The emergence of COVID-19 has required a re-prioritization of healthcare resources in many dimensions. Cancer is a leading cause of death in the developed world, and cancer patients have been particularly impacted by the COVID-19 pandemic. Early studies from Wuhan suggest that patients with cancer are at greater risk of acquiring coronavirus and also death from subsequent COVID-19 infections1, 2. Clinicians have therefore tried to minimize risk of infection among newly diagnosed cancer patients by delaying time until treatment for certain patients, or by modifying treatment standards for certain patients (e.g. for prostate cancer, offering a longer course of pre-treatment hormone therapy prior to initiation of radiation therapy).
Given the potential of COVID-19 to infect both patients and staff members, cancer facilities are currently triaging the care of cancer patients and adjusting the time until treatment initiation (TTI). This prioritization is consistent with guidelines from the Centers for Disease Control and Prevention that recommend that health care providers give priority to urgent and emergency visits and procedures3. Even prior to the current pandemic, TTI had been trending upward—from 21 in 2004 to 29 days in 2013—among cancer patients primarily because of the increasing complexity of care 4. Yet, most of the decisions about how to triage patients have been made without the benefit of a solid evidence base or guidelines.
The American Society of Clinical Oncology recently published guidelines on how the care of patients with cancer should be modified by the COVID-19 pandemic 5. Curiously missing from these guidelines, however, are specific recommendations for modifying care, including an optimal TTI. This is not entirely surprising, as very little is known about the novel coronavirus and there is a very small evidence base for practice guidelines. For example, there is no consensus regarding (1) the primary disease sites (e.g., prostate, breast) for which TTI may be safely prolonged, (2) cancer stages for which TTI may be safely prolonged, and (3) the appropriate duration of TTI for particular treatment modalities (e.g., radiation therapy, chemotherapy, surgery, hormone therapy) without impacting survival.
There are several studies that have investigated TTI outside of the COVID-19 context, with mixed results. For example, Khorana et al. studied TTI for surgery, radiotherapy, or chemotherapy, among six specific cancers 4. They found that increased TTI was associated with poorer survival for stage I and II breast, lung, renal and pancreatic cancers, and stage I colorectal cancers, with increased risk of mortality ranging from 0.5% to 3% for each week of delay. Murphy et al. studied delay of chemoradiotherapy for head and neck cancer and found that a TTI of <67 days was ideal 6, 7. Similarly, for colon cancer, each additional week of delay was shown to be associated with 7% lower survival 8. Among women with breast cancer, delay of chemotherapy or surgery was found to be associated with lower survival 9, 10. On the other hand, increased TTI does not appear to have negative impact on survival for certain patients with cervical or pancreatic cancer 11, 12, 13. A forthcoming study by Turaga and Girotra studied delaying surgical treatment for twenty-one cancers and suggested that most surgeries can safely be delayed for four weeks 14. The few studies that have been done suggest that treatment for some cancers and stages can be safely delayed, while treatment for others cannot be delayed without risking a significantly poorer outcome for the patient.
Opportunities
While these prior studies are informative, there are gaps that have an urgent need to be filled in order to effectively face the resource limitations of the current pandemic. These gaps also suggest a framework for a research agenda. Prior studies have generally focused on a single cancer site, stage, and treatment, yet the current need calls for a broad, comprehensive evaluation that considers as wide a range of disease sites and stages and their most common treatment approaches as possible. Our own current work is using available data that contains natural variations in TTI in order to fill these gaps in the evidence base.
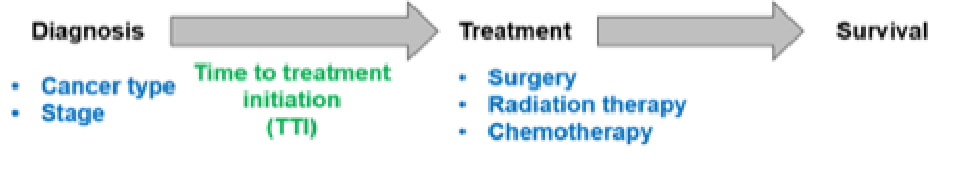
We are currently evaluating the impact of increasing TTI as a function of disease site, stage, and treatment modality for the thirty most prevalent cancers, across four stages, and for three broad treatment strategies (Figure 1). Our central hypotheses are that (1) increasing TTI will have a greater negative impact on survival for certain sites than for others; (2) patients with stage I-II disease will have the greatest benefit of a lower TTI vs stage III-IV; and (3) increasing TTI with any treatment modality will have a negative impact on survival. Based on our findings we will develop a cancer treatment triage protocol prioritizing particular treatment modalities for certain cancer types based on stage.
If the US experience of COVID-19 is similar to the experience in Europe and China, the impact of COVID-19 can be expected to last for at least 6-12 months 15. During this time, delay and disruption of care for patients with cancer is inevitable. Cancer cases will be triaged, and diagnosis of new cancers will continue. The overarching goal of our work is to assure that clinicians have the information they need in order to balance the trade-off between exposure and delay. Our work will show which cancer sites and stages can be safely delayed, and for how long, and which cancer sites and stages have risks to delay that outweigh the risk of COVID-19 exposure.
- 1Liang W, Guan W, Chen R, Wang W, Li J, Xu K, et al. Cancer patients in SARS-CoV-2 infection: a nationwide analysis in China. The Lancet Oncology. 2020;21(3):335-7. Epub 2020/02/19. https://doi.org/10.1016/s1470-2045(20)30096-6. PubMed PMID 32066541
- 2Yu J, Ouyang W, Chua MLK, Xie C. SARS-CoV-2 Transmission in Patients With Cancer at a Tertiary Care Hospital in Wuhan, China. JAMA oncology. 2020. Epub 2020/03/27. https://doi.org/10.1001/jamaoncol.2020.0980. PubMed PMID 32211820; PubMed Central PMCID PMC7097836.
- 3Centers for Disease Control and Prevention. Coronavirus Disease 2019 (COVID-19): For Healthcare Professionals Atlanta: CDC; 2020 [cited 2020 April 1, 2020]. Available from: https://www.cdc.gov/coronavirus/2019-ncov/hcp/index.html?CDC_AA_refVal=…
- 4a4bKhorana AA, Tullio K, Elson P, Pennell NA, Grobmyer SR, Kalady MF, et al. Time to initial cancer treatment in the United States and association with survival over time: An observational study. PloS one. 2019;14(3):e0213209. Epub 2019/03/02. https://doi.org/10.1371/journal.pone.0213209. PubMed PMID 30822350; PubMed Central PMCID PMC6396925.
- 5American Society for Clinical Oncology. COVID-19 Patient Care Information Alexandria: ASCO; 2020 [cited 2020 April 1, 2020]. Available from: https://www.asco.org/asco-coronavirus-information/care-individuals-canc….
- 6Murphy CT, Galloway TJ, Handorf EA, Egleston BL, Wang LS, Mehra R, et al. Survival Impact of Increasing Time to Treatment Initiation for Patients With Head and Neck Cancer in the United States. Journal of clinical oncology : official journal of the American Society of Clinical Oncology. 2016;34(2):169-78. Epub 2015/12/03. https://doi.org/10.1200/jco.2015.61.5906. PubMed PMID 26628469; PubMed Central PMCID PMC4858932.
- 7Murphy CT, Galloway TJ, Handorf EA, Wang L, Mehra R, Flieder DB, et al. Increasing time to treatment initiation for head and neck cancer: an analysis of the National Cancer Database. Cancer. 2015;121(8):1204-13. Epub 2014/12/11. https://doi.org/10.1002/cncr.29191. PubMed PMID 25490875.
- 8Sun Z, Adam MA, Kim J, Nussbaum DP, Benrashid E, Mantyh CR, et al. Determining the Optimal Timing for Initiation of Adjuvant Chemotherapy After Resection for Stage II and III Colon Cancer. Diseases of the colon and rectum. 2016;59(2):87-93. Epub 2016/01/07. https://doi.org/10.1097/dcr.0000000000000518. PubMed PMID 26734965.
- 9Kupstas AR, Hoskin TL, Day CN, Habermann EB, Boughey JC. Effect of Surgery Type on Time to Adjuvant Chemotherapy and Impact of Delay on Breast Cancer Survival: A National Cancer Database Analysis. Annals of surgical oncology. 2019;26(10):3240-9. Epub 2019/07/25. https://doi.org/10.1245/s10434-019-07566-7. PubMed PMID 31332635.
- 10Bleicher RJ, Ruth K, Sigurdson ER, Beck JR, Ross E, Wong YN, et al. Time to Surgery and Breast Cancer Survival in the United States. JAMA oncology. 2016;2(3):330-9. Epub 2015/12/15. https://doi.org/10.1001/jamaoncol.2015.4508. PubMed PMID 26659430; PubMed Central PMCID PMC4788555.
- 11Ramey SJ, Asher D, Kwon D, Ahmed AA, Wolfson AH, Yechieli R, et al. Delays in definitive cervical cancer treatment: An analysis of disparities and overall survival impact. Gynecologic oncology. 2018;149(1):53-62. Epub 2018/04/02. https://doi.org/10.1016/j.ygyno.2017.12.010. PubMed PMID 29605051.
- 12Mirkin KA, Greenleaf EK, Hollenbeak CS, Wong J. Time to the initiation of adjuvant chemotherapy does not impact survival in patients with resected pancreatic cancer. Cancer. 2016;122(19):2979-87. Epub 2016/06/22. https://doi.org/10.1002/cncr.30163. PubMed PMID 27328270.
- 13Mirkin KA, Hollenbeak CS, Wong J. Time to Surgery: a Misguided Quality Metric in Early Stage Pancreatic Cancer. Journal of gastrointestinal surgery : official journal of the Society for Surgery of the Alimentary Tract. 2018;22(8):1365-75. Epub 2018/03/10. https://doi.org/10.1007/s11605-018-3730-0. PubMed PMID 29520648.
- 14Turaga KK, Girotra S. Are we harming cancer patients by delaying their cancer surgery during the COVID-19 pandemic? Ann Surg In Press.
- 15Remuzzi A, Remuzzi G. COVID-19 and Italy: what next? Lancet (London, England). 2020. Epub 2020/03/18. https://doi.org/10.1016/s0140-6736(20)30627-9. PubMed PMID 32178769; PubMed Central PMCID PMC7102589.






